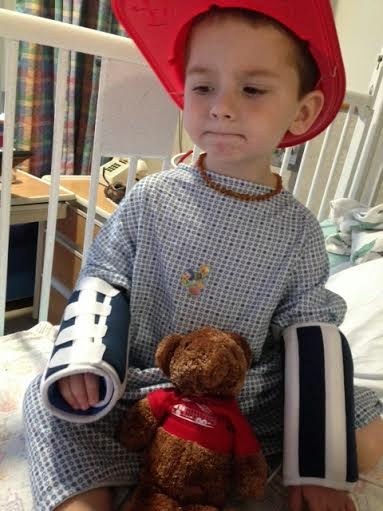
It's been a better week. I feel like I've accomplished more, anyway. I've made strides toward getting Aidan where he needs to be.
The Diagnostic and Complex Care Team reviewed Aidan's chart and called to set up his consult with Dr. Magnusson. I don't know whether this means it's a visit to decide whether they'll take Aidan on, or it's the first step in the process of having Dr. Magnusson on our side. Either way, it's a step in the direction we so desperately need, and it isn't even that far off (October 23rd). I've heard truly amazing things about this doctor - that he's amazing to have on your side, that he's smart and he'll fight for you, get you what you need, and put you in your place when need be. All of that and more - and we need it all so badly. I'm looking forward to the appointment, but I also know that I need to seriously organize my thoughts before then. I need to be armed with a clear and concise history and how and where we need his help.
I've also been continuing to talk with Children's Hospital of Pittsburgh's Center for Rare Disease Therapy (Rare Care). I am working with CHOP to gather Aidan's medical records, and once I have them and can get them to Rare Care, we'll be able to figure out exactly which doctors Aidan needs to see there. I've faxed the requests over to CHOP's records department, so now I wait. I have no idea how long it will take for CHOP to gather and mail his records to me. I'm oddly curious to see them, actually. But mostly, I'm anxious to get them to Rare Care so we can get the ball rolling. They have appointments available in November, but think that if we can get his records over quickly, they may be able to squeeze him in sooner. November would be great. Sooner would be amazing.
All of this is so much more direction than we had even two weeks ago.
On the home front, sleep has been hard to come by this week. I think Aidan's been sleeping more restlessly than usual - we've had two accidental unhookings overnight, and when we check on him overnight, he seems especially entangled lately. A few nights ago, we were all awoken at 4:30am to a low blood sugar, high ketone boy. He was cold and clammy and had been vomiting repeatedly in bed - all because his extension popped out and we fed the bed. Totally commonplace in the feeding tube world, but very dangerous for a hypoglycemic kiddo.
On a fun note - Aidan got to spend time with his bestie over the weekend. It will never stop warming my heart to see him just get to be a little boy. These boys have so much to teach each other. I love that T pushes Aidan to try bigger, braver, better things. I love that Aidan shows T that it's okay for everyone to do things in their own time, at their own speed. I love that they can both learn how to meet a friend where he is, even if that's not where you are. T is a sweet boy with a sensitive heart who has loved Aidan like a brother since birth. We are so lucky to know him.
He also (creative boy!) had a great time making a robot that could do all of his smiling for him. Maybe I've been irritating him too much, asking him to smile for pictures? He was so proud of his robot's big smile, and said that now HE doesn't have to smile. Great problem-solving, little Vulcan. So proud :)
All in all, it's been a better week. Over the next week, I'm hoping for more communication with Rare Care, a special Mommy/Aidan date on Labor Day, and my first time at a special needs parent support group - something that's been FAR TOO LONG in coming.
The Diagnostic and Complex Care Team reviewed Aidan's chart and called to set up his consult with Dr. Magnusson. I don't know whether this means it's a visit to decide whether they'll take Aidan on, or it's the first step in the process of having Dr. Magnusson on our side. Either way, it's a step in the direction we so desperately need, and it isn't even that far off (October 23rd). I've heard truly amazing things about this doctor - that he's amazing to have on your side, that he's smart and he'll fight for you, get you what you need, and put you in your place when need be. All of that and more - and we need it all so badly. I'm looking forward to the appointment, but I also know that I need to seriously organize my thoughts before then. I need to be armed with a clear and concise history and how and where we need his help.
I've also been continuing to talk with Children's Hospital of Pittsburgh's Center for Rare Disease Therapy (Rare Care). I am working with CHOP to gather Aidan's medical records, and once I have them and can get them to Rare Care, we'll be able to figure out exactly which doctors Aidan needs to see there. I've faxed the requests over to CHOP's records department, so now I wait. I have no idea how long it will take for CHOP to gather and mail his records to me. I'm oddly curious to see them, actually. But mostly, I'm anxious to get them to Rare Care so we can get the ball rolling. They have appointments available in November, but think that if we can get his records over quickly, they may be able to squeeze him in sooner. November would be great. Sooner would be amazing.
All of this is so much more direction than we had even two weeks ago.
On the home front, sleep has been hard to come by this week. I think Aidan's been sleeping more restlessly than usual - we've had two accidental unhookings overnight, and when we check on him overnight, he seems especially entangled lately. A few nights ago, we were all awoken at 4:30am to a low blood sugar, high ketone boy. He was cold and clammy and had been vomiting repeatedly in bed - all because his extension popped out and we fed the bed. Totally commonplace in the feeding tube world, but very dangerous for a hypoglycemic kiddo.
 |
| This has to be a strangulation hazard - right? |
 |
| Best Friends go with it when you rename their clubhouse "The Charmed House" |
He also (creative boy!) had a great time making a robot that could do all of his smiling for him. Maybe I've been irritating him too much, asking him to smile for pictures? He was so proud of his robot's big smile, and said that now HE doesn't have to smile. Great problem-solving, little Vulcan. So proud :)
All in all, it's been a better week. Over the next week, I'm hoping for more communication with Rare Care, a special Mommy/Aidan date on Labor Day, and my first time at a special needs parent support group - something that's been FAR TOO LONG in coming.